Services We offer
- Uterine Fibroids
- Pelvic Pain
- Polycystic Ovary Syndrome
- Ovarian Cysts
- Recurrent Miscarriage
- Laparoscopic Hysterectomy
- Laparoscopic Myomectomy
- Heavy Uterine Bleeding
- Geriatric Gynecology
- Endometriosis Surgery
- Adenomyosis
- Recanalization
- Hysteroscopic Myomectomy
- Ectopic Pregnancy
- Fertility Promoting Surgery

Pelvic Pain
WHAT IS PELVIC INFLAMMATORY DISEASE?
Pelvic inflammatory disease (PID) is a serious bacterial infection that can occur anywhere in the upper genital /reproductive tract (uterus, fallopian tubes and ovaries). PID can develop from normal vaginal or cervical bacteria or result from a sexually transmitted disease (STD). STD’s chlamydia and gonorrhea, the two most common bacterial causes of PID, if left untreated, can result in adhesions (scarring) within the fallopian tubes, uterine lining, ovaries or other abdominal areas. Fallopian adhesions can lead to infertility and increased incidence of ectopic pregnancy, where a fetus develops outside of the uterus and which can be life threatening.

Pelvic Pain Treatment in Kolkata
Bacteria causing PID can spread upward from the vagina or cervix (opening to the uterus) into the fallopian tubes, ovaries, uterus and into the abdominal cavity. PID can take anywhere from several days to several months to develop. Untreated PID infections may lead to infertility, cystitis (inflammation of the bladder), ectopic (tubal) pregnancy, recurrent episodes of PID and chronic pelvic pain.Sexually active women between the ages of 15 and 25 have the highest incidence of PID.
WHAT CAUSES PID TO SPREAD?
• Using an intrauterine device (IUD). (The risk of infection is greatly diminished when a woman is tested and treated for PID before an IUD insertion).
• Natural bacteria development
• Women who douche once or twice a month are more likely to have PID than those who douche less than once a month. Douching may flush bacteria into the uterus, ovaries and fallopian tubes, causing infection, and may ease symptoms of PID, thus delaying effective treatment.
• Previous pelvic infections. A prior episode of PID increases the risk of another episode, since the body’s defenses are often damaged during an initial bout of PID.
• Gonorrhea causing PID may gain access more easily during menstruation, if blood carrying organisms flows backward from the uterus into the fallopian tubes.
WHAT ARE THE SYMPTOMS OF PID?
PID associated symptoms may range from mild to severe. A woman with PID causing chlamydia may show no or mild effects. However, PID does have a wide range of symptoms.
• Dull or intense pain, usually affecting both sides of the lower abdomen or back.
• Lower abdominal and back pain not associated with a period is often one of the first signs of PID reported by patients.
• Tenderness of the uterus, ovaries and fallopian tubes during the pelvic exam
• Burning or pain during urination
• Nausea and vomiting
• Bleeding between menstrual periods
• Increased or changed vaginal discharge, that may have a foul odor
• Painful sexual intercourse
• Rectal pain
• Fever and chills
DIAGNOSING PID
PID is often difficult to diagnose because the symptoms can be mild. It is possible for a woman to have PID and be asymptomatic (without symptoms) or have symptoms too mild to notice for an unknown period of time. PID can also be misdiagnosed as appendicitis, ruptured ovarian cysts or other problems.
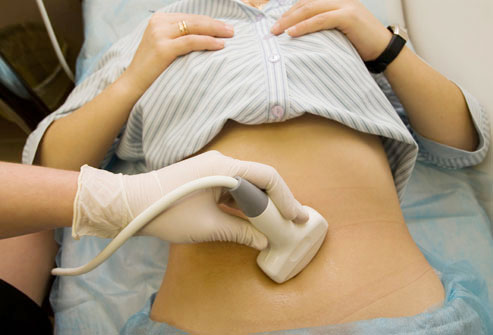
A physician will perform a complete exam, including a gynecologic, sexual and menstrual history, a fever, vaginal and cervical discharge check and a test for gonorrhea and chlamydia. All patients of childbearing age with lower abdominal pain will require a pregnancy test to rule out an ectopic pregnancy. Cervical and vaginal samplings will be taken for cancer and microbes screening. A rectal exam will be performed to evaluate the pelvic area behind the uterus. If more information is necessary, the doctor may order other tests, such as ultrasound to view whether the fallopian tubes are enlarged or an infection is present, endometrial biopsy or laparoscopy to distinguish between PID and other serious problems. Laparosopy is both a diagnostic and surgical procedure in which a tiny flexible tube with a light is inserted through a small incision or incisions just below the navel. This step allows the doctor to view the internal abdominal and pelvic organs as well as take specimens for cultures or microscopic studies if necessary.
Any woman who has had a new sexual partner, multiple partners or unprotected sex should be screened regularly for PID. A detailed sexual history is essential to assess the risk for PID.
PID AND INFERTILITY
PID causing bacteria can infect or cause inflammation or scarring of the fallopian tubes. These tubes can become totally blocked with scar tissue, causing infertility. However, fallopian tubes do not have to be totally blocked for a fertilized egg to get stuck in the tube, where it can begin to grow like in the uterus. This is called an ectopic pregnancy, which can cause the tube to rupture or break open and result in severe pain, internal bleeding and even death. The longer a woman waits to get treatment for PID, the more likely she is to become infertile.
PID TREATMENT OPTIONS
Early treatment may prevent the development of PID, especially in screening women who unknowingly had Chlamydia infection. PID can be treated as follows:
• Two oral antibiotics are generally prescribed at the same time. A woman should abstain from sexual intercourse until she has finished her medications and her followup exams have been successfully completed
• Antimicrobial agents to treat gonorrhea, chlamydia, streptococci and other gram-negative bacteria are prescribed
• Sex partners of patients who have PID should be examined and treated, if they have had recent sexual contact, to avoid re-infection
PID TREATMENT FOLLOW-UP
Follow-up with a physician is an important part of the PID therapy, which requires that a woman:
• Take and complete all medications as directed
• Attend follow-up visits to make sure medicine is working
• Be examined following treatment completion to make certain infection is gone
• Tell partner to get tested and treated
• Refrain from sex until patient and partner have been treated and cured
Some women with suspected PID need to be hospitalized if they are severely ill, require intravenous antibiotics, are pregnant, the diagnosis is uncertain, require treatment for an abdominal emergency, such as a appendicitis, or are infected with HIV.Untreated PID can cause chronic pelvic pain and scarring – conditions which are difficult to treat but are sometimes improved with surgery. Surgery is generally not utilized to treat PID, but a woman experiencing chronic PID with pelvic pain may speak with her doctor about surgically removing the damaged or infected reproductive organs. The procedures noted below are surgical treatment options for women with chronic PID:
• Salpingectomy is the removal of one or both fallopian tubes, but will only stop PID if infection is confined to the tube(s). PID may still spread to other pelvic areas. However, if both tubes are removed, natural pregnancy will be prevented.
• Hysterectomy, abdominal or vaginal, is the removal of the uterus and possibly the cervix. This procedure may reduce PID and accompanying pelvic pain, but there isno guarantee if PID scarring has spread outside of the womb. Following this procedure, a woman will not be able to have children.
• Oophorectomy is the removal of one or both ovaries and may be performed with a hysterectomy. This procedure results in menopausal symptoms.
• Adhesiolysis involves laparoscopic removal of tube blocking scar tissue. Operative laparoscopy is used to treat pelvic inflammatory disease, specifically scar tissue and tubal obstruction.
PID PREVENTION
Establishing safe sex practices is the foundation of PID prevention.
• Abstain from sex
• Correctly use latex condoms for vaginal, oral and anal sex from the start of sexual contact. Be aware that condoms don’t provide complete protection against STD’s and that birth control pills, shots, implants or diaphragms won’t protect a woman from STD’s
• Maintain mutual monogamy
• Attend regular checkups if sexually active
• Refrain from sex until all partners have been treated and cured for STD’s
• Use water-based spermicides, along with latex condoms, for additional protection during vaginal intercourse
• Avoid douching
• Sex partner should be treated even if he or she does not have symptoms
CONCLUSION
It is important to talk to your partner as soon as possible if you have an STD, so he or she can get treatment. Also talk to your doctor or nurse about whether or not you should be tested. The quicker you seek treatment the less likely the STD will cause you severe harm and the sooner you tell your sex partners about having an STD, the less likely they will spread the disease to other.